Laparoscopic Gastric Bypass
Laparoscopic gastric bypass is a weight loss or ‘bariatric’ procedure which can help patients who are significantly obese* (laparoscopic surgery is commonly known as ‘keyhole’ or ‘minimally invasive’ surgery).
The difficulty with obesity from a medical perspective is its association with a range of serious metabolic conditions, including…
- Diabetes.
- High blood pressure.
- Obstructive sleep apnoea.
- High cholesterol / high triglycerides.
- Infertility.
- Polycystic ovarian syndrome.
Surgical approaches are generally only recommended where other non-surgical weight loss methods have not worked. In some cases, a laparoscopic gastric bypass can be reversed.
Laparoscopic gastric bypass is really a name to describe three different operations. And some of those operations have more than one name, so it can be confusing. Let me try to simplify.
Gastric bypass in whatever form means a reduction in the size of the stomach by stapling or removing part of this organ, plus a change in the ability of the small bowel to absorb nutrients such as protein, calories, fats and vitamins (called ‘malabsorption’). The normal length of the small bowel can vary between 3-10 metres. The amount of small bowel which is bypassed varies between operations.
So, this malabsorption means that less food is absorbed but there is a risk of too much malabsorption. This could possibly mean protein and other deficiency, including calcium and changes to bones. This means that it is essential that the patient having a bypass operation remains on nutritional supplementation and under dietary review, forever.
Indications
See the indications section for laparoscopic gastric banding as substantially the same conditions apply for the procedures described here. A gastric bypass is sometimes recommended where a previous gastric banding procedure has not resulted in weight loss.
Types of Bypass Procedures
Roux-En-Y Gastric Bypass (‘RYGB’)
This is the traditional bypass but perhaps now becoming less popular due to risks such as dumping syndrome, low blood sugar and an internal hernia (which requires an emergency operation). The stomach is made smaller but not removed.
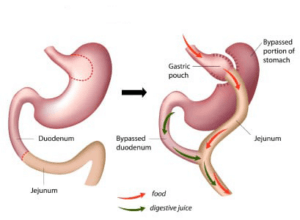
Loop Gastric Bypass
This operation has several other names. (Omega Loop, Single Anastomosis Gastric Bypass, One Anastomosis Gastric Bypass). The stomach is made smaller but not removed. There is one joint from stomach to bowel. The risks of internal hernia are lower than RYGB but there are still small risks of an ulcer and reflux.
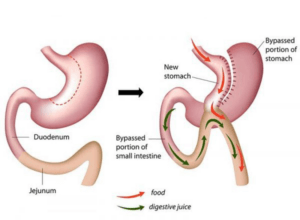
SIPS SADI
This is essentially a sleeve gastrectomy and, at the same time or at a later date, a bypass operation. The difference between this and the loop bypass is that a portion of the stomach is removed and that the bypass is from the duodenum to small bowel and not stomach to small bowel. This is reported to reduce the risk of an ulcer and reflux. This is a relatively new operation and the long-term consequences are uncertain.
Bypass Procedure
A gastric bypass is generally conducted via laparoscopic (‘keyhole’/’minimally invasive’) surgery. Between four and six small incisions are made to the abdomen to allow the miniaturised surgical instruments to be inserted in the abdominal cavity. The surgeon is able to visualise the procedure via a small video camera. The operation is conducted under a general anaesthetic and normally takes between two and four hours to complete.
Risks
All surgical procedures carry some degree of risk, and some of these are common to all invasive procedures. These include risks relating to the anaesthetic, bleeding and wound infection.
There are some specific complications that may arise after gastric bypass surgery. These are…
- Staple line leak.
- Thrombosis (the formation of a blood clot).
- Inflammation to, or blockage of the opening to the stomach (‘stricture’).
The following conditions may also develop after the procedure…
- Gallstones.
- Nutritional deficiency.
- Gastro-Oesophageal Reflux Disease (‘GORD’).
Most of these risks and complications are uncommon and Dr Watson will be able to answer any questions you have prior to undergoing a gastric bypass procedure.
What procedure is best for me?
When you meet Dr Watson, he will discuss the various options and work with you to determine which operation may be the best for your individual situation. This may depend on factors such as your Body Mass Index (BMI), whether you are diabetic, previous surgery and expectations.